Healthcare has always been a very personal and interactive industry, with huge importance placed on building a rapport, and having face to face contact with your patients. However, changes in society and technology are increasingly morphing this dynamic as more and more emphasis is placed on patients’ monitoring and controlling their conditions at home.
An ageing population in the UK and the rise of chronic conditions has placed unique pressures on our healthcare system, as patients no longer want the stress of repeated hospital appointments. Patients can’t be bothered with time wasting trips to their GP or local hospital, especially if they have mobility problems, however many are also very clued up on their conditions, and are therefore keen to keep track of things themselves.
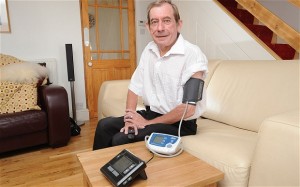
Bringing healthcare home
The home is slowly becoming a more usual area to receive healthcare, and technology is becoming a vital aspect of this with new teleheath initiatives letting engaged patients keep an eye on their conditions without the strain of a trek to the hospital. An example of this would be More Independent, a scheme introduced by the Liverpool Clinical Commissioning Group.
Dave Horsfield, programme manager, emphasises that healthcare at home is far from isolating. “Patients who regularly monitor their condition alongside the support of a health professional feel more confident, and can therefore get out and about in their community more,” he said.
Although the older generation aren’t exactly famed for being techno savvy, Mr Horsfield claims this hasn’t been a problem so far, with help readily available for those who need it. With the shift from hardware to software becoming more evident however, one of the key issues will be that technology is always changing, adapting and progressing, meaning that any telehealth programme will also have to constantly evolve to keep up. The NHS has so far dealt with this by leasing equipment instead of selling or giving as it is more flexible.
Less upheaval
“For many patients it’s meant less stress and upset for them and their families, as well as reduction in unplanned visits to the GP or hospital,” Mr Horsfield explains. As well as the decrease in emotional upset, telehealth has also been proven to be cheaper despite the outlay of equipment. The patients experience better outcomes as their symptoms are more closely watched, but the overall cost of telehealth is also lower than the avoided admissions price. Telehealth could even enable some patients to engage in their treatments at home, for example non-invasive ventilation and sleep therapy, which professionals can then review and get in touch with the patient if they have any concerns about the results.

Another plus point of telehealth is the ability to create a really in-depth and comprehensive care plan that caters directly to your patient and includes elements of self-monitoring. A patient’s weight, blood pressure, pulse and change in symptoms can be tracked closely from the comfort of their own homes, although it has been acknowledged that some conditions are too unstable for remote monitoring.
Broadening the scheme
With initial positive results, plans to upscale the telehealth project have been discussed, however working out how to cover larger numbers of patients and adapt working practices among staff are easier said than done. Some schemes have used a call centre style approach, with staff going through results before notifying a nurse.
Although ironing out the wrinkles of implementing a telehealth system may require some juggling, Sara Parsons, who runs a sleep service at St George’s Hospital in London, hits the nail on the head when she identifies the main benefit of using telehealth: “The big thing for me is being able to deal with issues as they crop up, rather than waiting. Some patients used to struggle for several weeks between appointments.”
What do you think about potentially using telehealth? Is this something you would use at home?


